http://jcem.endojournals.org/content/82/11/3793.full
Comparison of self-assessment of libido at the 2 year point showed a dramatic improvement in the testosterone group compared to that in the controls (Fig. 1⇓). The incidence of new illnesses during the course of the study was not significantly different in the two groups for coronary artery disease, peripheral vascular disease, myocardial infarctions, angina, diabetes mellitus, or transient ischemic attacks (Table 3⇓). Benign prostatic hypertrophy (BPH) has long been a concern associated with long term testosterone administration. This study found that the control group had a higher rate of BPH than the study group, but the difference was not statistically significant.
The 2 yr changes in serum and hematocrit values of the two groups are compared in Table 2⇓. There were no significant differences in the prostate-specific antigen concentration. The urea nitrogen to creatinine ratio dropped in the study group, but the change was not statistically significant. Only hematocrit showed a significant increase in the testosterone-treated group compared to that in controls. Eleven subjects (24%) in the testosterone group developed polycythemia (hemoglobin, >17 g/dL; hematocrit, >52%), warranting temporary withdrawal of testosterone therapy or phlebotomy. Of these, the first occurrence of polycythemia was within the first year of therapy in six (33%) subjects, between 1–2 yr in 3 (6.7%) subjects, and beyond 2 yr in two (4.4%) subjects.
Latest clinical and research information on men's health. Type your question in the following box:
Search This Blog
Translate
Showing posts with label prostate. Show all posts
Showing posts with label prostate. Show all posts
Saturday, December 29, 2012
Sunday, December 9, 2012
Testosterone Therapy in Men With Prostate Cancer: Scientific and Ethical Considerations
Morgentaler A. Testosterone Therapy in Men With Prostate Cancer: Scientific and Ethical Considerations. The Journal of Urology 2013;189(1, Supplement):S26-S33. http://www.sciencedirect.com/
P
urpose Pertinent literature regarding the potential use of testosterone therapy in men with prostate cancer is reviewed and synthesized.
Materials and Methods A literature search was performed of English language publications on testosterone administration in men with a known history of prostate cancer and investigation of the effects of androgen concentrations on prostate parameters, especially prostate specific antigen.
Results The prohibition against the use of testosterone therapy in men with a history of prostate cancer is based on a model that assumes the androgen sensitivity of prostate cancer extends throughout the range of testosterone concentrations. Although it is clear that prostate cancer is exquisitely sensitive to changes in serum testosterone at low concentrations, there is considerable evidence that prostate cancer growth becomes androgen indifferent at higher concentrations. The most likely mechanism for this loss of androgen sensitivity at higher testosterone concentrations is the finite capacity of the androgen receptor to bind androgen. This saturation model explains why serum testosterone appears unrelated to prostate cancer risk in the general population and why testosterone administration in men with metastatic prostate cancer causes rapid progression in castrated but not hormonally intact men. Worrisome features of prostate cancer such as high Gleason score, extracapsular disease and biochemical recurrence after surgery have been reported in association with low but not high testosterone. In 6 uncontrolled studies results of testosterone therapy have been reported after radical prostatectomy, external beam radiation therapy or brachytherapy. In a total of 111 men 2 (1.8%) biochemical recurrences were observed. Anecdotal evidence suggests that testosterone therapy does not necessarily cause increased prostate specific antigen even in men with untreated prostate cancer.
Conclusions Although no controlled studies have been performed to date to document the safety of testosterone therapy in men with prostate cancer, the limited available evidence suggests that such treatment may not pose an undue risk of prostate cancer recurrence or progression.
Materials and Methods A literature search was performed of English language publications on testosterone administration in men with a known history of prostate cancer and investigation of the effects of androgen concentrations on prostate parameters, especially prostate specific antigen.
Results The prohibition against the use of testosterone therapy in men with a history of prostate cancer is based on a model that assumes the androgen sensitivity of prostate cancer extends throughout the range of testosterone concentrations. Although it is clear that prostate cancer is exquisitely sensitive to changes in serum testosterone at low concentrations, there is considerable evidence that prostate cancer growth becomes androgen indifferent at higher concentrations. The most likely mechanism for this loss of androgen sensitivity at higher testosterone concentrations is the finite capacity of the androgen receptor to bind androgen. This saturation model explains why serum testosterone appears unrelated to prostate cancer risk in the general population and why testosterone administration in men with metastatic prostate cancer causes rapid progression in castrated but not hormonally intact men. Worrisome features of prostate cancer such as high Gleason score, extracapsular disease and biochemical recurrence after surgery have been reported in association with low but not high testosterone. In 6 uncontrolled studies results of testosterone therapy have been reported after radical prostatectomy, external beam radiation therapy or brachytherapy. In a total of 111 men 2 (1.8%) biochemical recurrences were observed. Anecdotal evidence suggests that testosterone therapy does not necessarily cause increased prostate specific antigen even in men with untreated prostate cancer.
Conclusions Although no controlled studies have been performed to date to document the safety of testosterone therapy in men with prostate cancer, the limited available evidence suggests that such treatment may not pose an undue risk of prostate cancer recurrence or progression.
Labels:
prostate,
prostate cancer,
PSA
Tuesday, May 22, 2012
What the U.S. Preventive Services Task Force Missed in Its Prostate Cancer Screening Recommendation
The U.S. Preventive Services Task Force (USPSTF), a panel that does not include urologists or cancer specialists, has just recommended against prostate-specific antigen (PSA)-based screening for prostate cancer, stating that “screening may benefit a small number of men but will result in harm to many others” (1). Recognizing that prostate cancer remains the second-leading cause of cancer deaths in men, we, an ad hoc group that includes nationally recognized experts in the surgical and radiological treatment of prostate cancer, oncologists, preventive medicine specialists, and primary care physicians, believe that the USPSTF has underestimated the benefits and overestimated the harms of prostate cancer screening. Therefore, we disagree with the USPSTF's recommendation.
Friday, February 24, 2012
Testosterone Replacement in Men Treated for Prostate Cancer
These two paragraphs were taken from an excellent review on Medscape entitled "Testosterone in Hypogonadal Men Treated for Prostate Cancer: Testosterone Replacement in Men Treated for Prostate Cancer" by D. Landau; T. Tsakok; S. Aylwin and S. Hughes.
Testosterone replacement therapy after radical prostatectomy was the focus of Kaufman and Graydon's study in seven patients with hypogonadism over a maximum follow-up period of 12 years. They reported symptomatic improvement of hypogonadism, with no evidence of cancer recurrence. Agarwal and Oefelein administered TRT to a similar group of 10 patients and also reported that no PSA recurrences were associated with rises in mean serum testosterone from 197 to 591 ng/dl. In a study by Khera et al.,57 men received testosterone for an average of 36 months following radical prostatectomy – no increases in PSA were seen over a mean follow-up of 13 months. Of note is the larger study by Sathyamoorthy et al. in 133 postprostatectomy patients, 21 (16%) of whom had either Gleason score ≥ 8, positive margins or nodes. There were no significant PSA rises associated with increases in mean testosterone levels from 262 to 418 ng/dl over a 1 year follow-up. A prospective study of 22 patients by Nabulsi et al. [reported that one patient (4·5%) experienced biochemical recurrence after TRT postradical prostatectomy.
Despite the intuitive concern that residual prostate tissue is more likely to result in residual microscopic disease susceptible to androgen stimulation, some studies evaluating the use of TRT after radiotherapy and brachytherapy have also produced encouraging data. Sarosdy[22]followed 31 men receiving testosterone after brachytherapy with a median 5 year follow-up, finding no incidence of cancer recurrence or progression. Morales et al. [looked at five men post external beam radiotherapy and noted marked symptomatic improvement, with no biochemical recurrence for up to 27 months. Davila et al. analysed PSA response after TRT in a split cohort of 20 patients after either prostatectomy or external beam radiation therapy. There were no biochemical recurrences and no differences between the two groups in PSA levels after testosterone replacement. Finally, Leibowitz et al reported a retrospective study of a heterogeneously treated population of 96 patients. 60% of participants had not received definitive local therapy and consequently had both malignant and benign prostatic tissue in situ; notably, 11 men in the study group had metastatic disease in remission after ADT. After a mean treatment duration of 15 months, 41 men (43%) had PSA progression. This high rate of PSA progression can in part be explained by the relatively high proportion of patients with aggressive disease (25% had Gleason score ≥ 8). However, it is also possible that stimulation of residual benign prostatic tissue contributed to the raised PSA levels, which in most cases returned to baseline following cessation of testosterone replacement. Elevated baseline PSA before testosterone replacement was associated with a significantly increased risk of PSA progression, serving as a reminder that this therapy should be restricted to patients in overt biochemical remission.
We have summarized a small number of mostly retrospective case series evaluating the safety of initiating TRT in postprostatectomy patients with negative margins and undetectable PSA levels. Overall, 42 of 381 (11%, range 0–43%) experienced biochemical recurrence, whilst the majority benefited from symptomatic improvement in their hypogonadism without adverse effects on PSA or tumour progression. It is likely that research in this field suffers from publication bias as well as the modest quality of most studies. Nevertheless, the data presented here are largely at odds with the longstanding taboo regarding the use of androgens in men with prostate cancer and again raises the question: is it of clinical consequence if a normal serum testosterone level is achieved in a prostate cancer survivor by natural or pharmacological means? Until more studies have been published on this subject, we should take a cautious and conservative approach.
Friday, October 28, 2011
Monitoring Testosterone Replacement Therapy (TRT)
Monitoring Testosterone Replacement Therapy (TRT)
| by Nelson Vergel Nelson Vergel is the author of "Testosterone: A Man's Guide  Excerpted from "Testosterone: A Man's Guide Excerpted from "Testosterone: A Man's GuideTestosterone replacement therapy is not without side effects, although most are manageable. I’ve been taking testosterone replacement for 16 years and for the most part have had few side effects thanks to careful monitoring. It’s critical that you are monitored for side effects in addition to your testosterone level. Some men may experience one or more side effects that sometimes go unnoticed until it is too late. In part it is the underground, unmonitored use of testosterone that creates so much bad publicity for a very helpful product. The first step in the proper monitoring of replacement therapy is providing your doctor with a thorough medical history. Appendix A shows a simple and comprehensive medical history form (courtesy of Dr John Crisler, allthingsmale.com). Patients who would like to be proactive can fill out this form and give a copy to their doctor. It is expected that every doctor have a similar form, although most do not ask questions pertinent to sexual function or on the use of androgens. Let your doctor know about all the medications you take so that medication-induced sexual dysfunction can be ruled out before starting testosterone. I also strongly believe that if a patient goes to the doctor to obtain a Viagra, Cialis or Levitra prescription, the doctor should check the patient’s testosterone blood levels to ensure that it is not the root of the problem. Hypogonadal men may not respond as well to these drugs if their testosterone is not normalized first. Studies combining testosterone and oral sexual enhancement drugs have shown a synergistic effect on sexual benefits. The following suggested guidelines for monitoring testosterone replacement is recommended by several physician groups and practices: You should be evaluated after the first month of therapy to measure your testosterone blood levels. If your doctor doesn’t ask, let him know about your quality of life. Make sure your doctor is aware of your energy level, mood, and sexual function, as well as any potential side effects (tender breasts, urinary flow decrease, moodiness, and acne). Ensuring Prostate Health—No Link Found Between Androgen Levels and Risk for Prostate CancerThe prostate is a gland that is part of the male reproductive system. Its function is to store and secrete a slightly alkaline (pH 7.29) a milky fluid which usually constitutes 25-30% of the volume of the semen along with spermatozoa. This alkaline fluid seems to neutralize the acidity in the vagina, prolonging the life span of the sperm. Also, the prostate contains some smooth muscles that help expel semen during ejaculation. It also helps control the flow of urine during ejaculation.A healthy human prostate is classically said to be slightly larger than a walnut. In actuality, it is approximately the size of a kiwi fruit. It surrounds the urethra just below the urinary bladder and can be felt during a rectal exam. 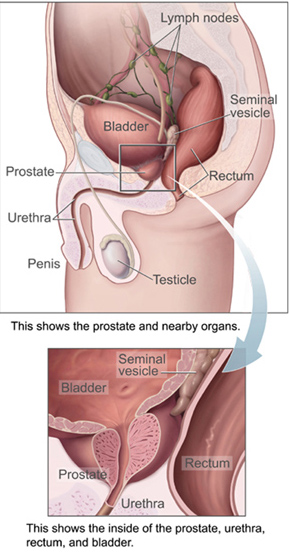 Prostate cancerThis little gland attracts a great deal of attention in men’s health. One of the major issues is related to cancer. Prostate cancer is one of the leading causes of death in men in the United States. As men age, small hidden prostatic lesions become increasingly common. These may or may not become cancerous. These lesions occur in 30 percent of American men over the age of 45, with the prevalence rising to more than 80 percent for men over the age of 80. Genetic factors and life style conditions such as diet are believed to contribute to this transformation. [Figure 14.The prostate and surrounding organs (Courtesy of Wikipedia.com)] Prostate cancerThis little gland attracts a great deal of attention in men’s health. One of the major issues is related to cancer. Prostate cancer is one of the leading causes of death in men in the United States. As men age, small hidden prostatic lesions become increasingly common. These may or may not become cancerous. These lesions occur in 30 percent of American men over the age of 45, with the prevalence rising to more than 80 percent for men over the age of 80. Genetic factors and life style conditions such as diet are believed to contribute to this transformation. [Figure 14.The prostate and surrounding organs (Courtesy of Wikipedia.com)]. Doctors use different methods to detect prostate cancer, including prostate-specific antigen (PSA) assays, digital rectal examination (DRE), and transrectal ultrasound. A DRE before starting testosterone replacement therapy and every six months is recommended, especially for men with a family history of prostate cancer or those older than 40 years. Nobody likes having a DRE but your continued good health is worth a few seconds of discomfort. An abnormal rectal exam, a confirmed increase in PSA greater than 2 ng/mL, or PSA of over 4 ng/mL will prompt a health care provider to refer you to a urologist for further evaluation (usually an ultrasound and prostate biopsies). Admittedly the PSA and the DRE lack sensitivity and specificity. 25 percent of patients with prostate cancer have normal PSA levels (false negatives), while benign prostatic hyperplasia (BPH), a non-cancerous inflammation, may elevate them (false positives). Researchers have found hidden prostatic lesions with needle biopsies in some men with normal PSA level and normal transrectal ultrasound findings. Prostate biopsies are part of routine clinical use of testosterone therapy and are not justified unless a sharp rise in PSA is observed and infections have been ruled out. There has some been confusion regarding testosterone replacement therapy’s role in PSA elevation or causing prostate cancer. Prostate cancer is initially androgen-dependent so testosterone therapy should not be used by men with prostatic cancer. This does not mean that it causes cancer. A huge pooled analysis of data from 18 studies (consisting of 3,886 men with prostate cancer and 6,438 controls), published in the February 6, 2008 issue of the Journal of the National Cancer Institute found that blood levels of androgens and other sex hormones do not seem to be related to an increased risk for prostate cancer. In short, testosterone therapy does not appear to cause prostate cancer but it can make it worse. Prostate infectionAnother health concern is prostatitis or prostate infection. This is common in aging men and can be a leading cause of an elevated PSA. Your doctor will want to check you for an infection if your PSA unexpectedly increases by checking your urine for white blood cells. If they are high, he may refer you to an urologist who would induce a discharge from your penis to look at it under the microscope. Don’t ask me how the urologist does it, ask the urologist! Benign prostatic hyperplasiaA common health condition is benign prostatic hyperplasia or BPH. It is estimated to occur in 50 percent of men older than 50 years. Increased frequency of urination, frequent trips to the bathroom at night, incomplete voiding, and urgency to urinate indicate possible prostatic inflammation. BPH does not necessarily lead to increased rates of prostate cancer. There have been no prospective, controlled, long-term studies on the effects of testosterone administration on either the development or the progression of BPH. One open label, one-year study that measured prostate size using ultrasound found no increase during testosterone replacement therapy, suggesting that the treatment does not cause BPH. Whether testosterone treatment worsens asymptomatic BPH has not been established. Some individuals are more prone to prostatic inflammation when using testosterone. Another study was conducted by Dr. Michael D. Trifiro at Moores UCSD Cancer Center in San Diego. Dr. Trifiro observed 158 men for 20 years to determine the correlation between serum sex hormones and lower urinary tract symptoms (reduced urinary flow, urgency, and other symptoms associated with BPH). The researchers found no significant associations of total testosterone, estradiol (E2)), testosterone: E2 ratio, DHT, or dehydroepiandrosterone with lower urinary track symptoms or with any measured hormones(published in BJU International in December 2009). Tesosterone replacement therapy is not contraindicated in those with BPH. Men with BPH who need to start testosterone replacement should be observed very closely. The first symptom that worsens with increased BPH is restricted urinary flow and urgency, especially during sleep hours. Many urologists are successfully prescribing medications to ease those symptoms and improve urinary flow in men with BPH. Finasteride (brand name: Proscar), which was approved by the FDA in 1992, inhibits production of dihydrotestosterone (DHT), which is involved with prostate enlargement. Its use can actually shrink the prostate in some men. However, many men using Proscar complain of erectile dysfunction (DHT receptors may be involved in healthy erctions). For men who experience this side effect, other medications may be of help. Proscar has also been found to decrease the risk of prostate cancer in men by 25 percent over aseven year period. More studies are ongoing. The FDA approved the drugs terazosin (brand name: Hytrin) in 1993, doxazosin (Cardura) in 1995, and tamsulosin (Flomax) in 1997 for the treatment of BPH. All three belong to the class of drugs known as alpha blockers. They work by relaxing the smooth muscle of the prostate and bladder neck to improve urine flow and to reduce bladder outlet obstruction. Terazosin and doxazosin were developed first to treat high blood pressure. Tamsulosin is the first alpha-blocker developed specifically to treat BPH. The main side effects of these drugs are nasal congestion, lowered blood pressure, and rash or itching. Most men using them report fast improvements in their urine flow within one to three days. They end up not having to get up in the middle of the night to urinate, so they sleep better and feel less fatigued during the day. The most common nonprescription agent used to alleviate symptoms of BPH is the over-the-counter herb saw palmetto (Serenoa repens). Extracted from the berry of the saw palmetto shrub, this substance is thought to inhibit 5-alpha reductase (5-·R), thus blocking the conversion of testosterone into DHT, which is responsible for stimulating growth of the prostate gland. Saw palmetto is generally well tolerated; side effects are infrequent, but include headache and gastrointestinal upset. No known drug interactions are associated with the use of this herb. Some studies found that saw palmetto led to an increase in urine flow rate in men with BPH compared with placebo, with effects comparable to finasteride. One randomized, double-blind, placebo-controlled study followed men with BPH who took standardized saw palmetto extract 160 mg or placebo twice daily for one year. There was no significant difference found between the saw palmetto and placebo groups in standardized objective urinary symptoms. The incidence of side effects was similar in the two groups. These results cast considerable doubt on the effectiveness of saw palmetto for the treatment of BPH. Patients who cannot tolerate BPH medications are now using emerging techniques like lasers to vaporize obstructing prostate tissue (www.greenlighthps.com). Talk to your urologist about this if you’re interested. PERSONAL COMMENT: After using testosterone for 17 years, I started to develop a weak urine flow. My doctor gave me prescriptions for several alpha blockers (Uroxatral, Flomax, etc). They worked great but I experienced a rash with each one. My urologist found a prostate infection, which he treated with antibiotics. The infection seemed to linger for months. I then received an ultrasound of my prostate. This test showed that my prostate was not enlarged. Instead it showed that a calcification, caused by a chronic prostatic infection, was blocking my urine flow through my prostate. I got the green light laser procedure done to open up my urethra. It worked great. So, what may seem like BPH may not be! Prostatic infections often go untreated for months since in many cases we may not have symptoms. Checking for Increased Blood Thickness (Polycythemia)In addition to increasing muscle and sex drive, testosterone can increase your body’s production of red blood cells. This hemopoietic (blood building) effect could be a good thing for those with mild anemia. An excessive production of red blood cells is called polycythemia; it’s not a good thing. With polycythemia the blood becomes very viscous or "sticky" making it harder for the heart to pump. High blood pressure, strokes, and heart attacks can occur. This problem is not that common in men taking replacement doses of testosterone but more common in those taking higher bodybuilder doses.It’s important to have your doctor check your blood’s hemoglobin and hematocrit.. Hemoglobin is the substance that makes blood red and helps transport oxygen in the blood. Hematocrit reflects the proportion of red cells to total blood volume. The hemoglobin and hematocrit should be checked before starting testosterone replacement therapy, at three to six months and then annually. A hematocrit of over 54 percent should be evaluated. Discontinuation of testosterone may be necessary but there is another option. Many patients on testosterone replacement who experience polycythemia do not want to stop the therapy due to fears of re-experiencing the depression, fatigue and low sex-drive they had before starting treatment. For those patients, therapeutic phlebotomy may be the answer. Therapeutic phlebotomy is very similar to what happens when donating blood, but this procedure is prescribed by your physician as a way to bring down your blood levels of hematocrit and viscosity. A phlebotomy of one pint of blood will generally lower hematocrit by about 3 percent. I have seen phlebotomy given weekly for several weeks bring hematocrit from 56 percent to a healthy 46 percent. I know physicians who prescribe phlebotomy once every six weeks because of an unusual response to testosterone replacement therapy. This simple procedure is done in a hospital blood draw facility and can reduce hematocrit, hemoglobin, and blood iron easily and in less than one hour. Unfortunately, therapeutic phlebotomy can be a difficult option to get reimbursed or covered by insurance companies. Your doctor may need to write a letter of medical necessity for it. If you are healthy and without HIV, hepatitis B, C, or other infections, you could also donate blood at a blood bank (a great way to help others!). The approximate amount of blood volume that needs to be withdrawn to restore normal values can be calculated by the following formula, courtesy of Dr. Michael Scally, an expert on testosterone side effect management. The use of the formula includes the assumption that whole blood is withdrawn. The duration over which the blood volume is withdrawn is affected by whether concurrent fluid replacement occurs. Volume of Withdrawn Blood (cc)= Weight (kg) × ABV×[Hgbi - Hgbf]/[(Hgbi +Hgbf)/2] ABV = Average Blood Volume (default = 70) Hgbi (Hcti) = Hemoglobin initial Hgbf (Hctf) = Hemoglobin final (desired); CC of blood volume to be withdrawn = 75 x 70 x [20 —l4]/[(20 + l4)/2] = 75 x 70 x (6/17) = approximately 1850cc; One unit of whole blood is around 350 to 450 cc; approximately 4 units of blood need to be withdrawn to decrease this man’s hemoglobin from 20 mg/mL to 14 mg/mL. The frequency of the phlebotomy depends on individual factors, but most men can do one every two to three months to manage their hemoglobin this way. Sometimes red blood cell production normalizes without any specific reason. It is impossible to predict exactly who is more prone to developing polycythemia, but men who use higher doses, men with higher fat percentage, and older men may have a higher incidence. Some doctors recommend the use of a baby aspirin (81 mg) a day and 2,000 to 4,000 mg a day of omega-3 fatty acids (fish oil capsules) to help lower blood viscosity and prevent heart attacks. These can be an important part of most people’s health regimen but they are not a replacement for therapeutic phlebotomy if you have polycythemia and do not want to stop testosterone therapy. It amazes me how many people assume that they are completely free of stroke/heart attack risks by taking aspirin and omega-3 supplements when they have a high hematocrit. Although some people may have more headaches induced by high blood pressure or get extremely red when they exercise, most do not feel any different when they have polycythemia. This does not make it any less dangerous. If you are using testosterone on your own you need to let your doctor know. Your physician may already suspect some sort of anabolic use if lab results reveal elevated hemoglobin and hematocrit. PERSONAL COMMENT: I had polycythemia back in the mid-1990s when I was using supraphysiologic doses of testosterone and nandrolone to reverse my HIV-related weight loss. I required two phlebotomies in six months. My hematocrit and hemoglobin eventually normalized without any reason even when using the same doses of testosterone and nandrolone. Ensuring Liver HealthI mentioned this before but it is well worth repeating. Contrary to what some physicians may think, injectable and transdermal testosterone have not been known to cause increased liver enzymes. The same cannot be said for over-the-counter supplements that claim to increase testosterone or growth hormone. Not only do most of them not work, but they could increase your liver enzymes to dangerous levels. This problem has been reported in the past to the FDA. I warn people all the time to be careful about their use. It is always good to check your liver enzymes when blood work is done since it is a cheap test and highly useful in detecting toxicities caused by medications or supplements you may be using.It is the use of oral testosterone and anabolic formulations (except for oral testosterone undecanoate, commonly used in Canada) that can increase liver enzymes. Many men with hepatitis B or C can be safely treated with replacement doses of testosterone without any liver injury if gels, patches or injections are used. I am very concerned that some of these patients may be denied this important therapy due to potential fears and misconceptions. Some studies have shown an increased incidence of hypogonadism, fatigue, and sexual dysfunction in patients with hepatitis. Some men like to take supplements to protect the liver against the damaging effects of medications, but very limited data is available on their use. Supplements potentially can interfere with medication blood levels; very little is known about supplement-drug interactions. However, I would like to bring up some supplements with data on liver protection:
Monitoring Blood PressureHigh blood pressure or hypertension is another serious medical condition that can go undetected because it often has no symptoms. It’s referred to as "the silent killer" for this reason. High blood pressure can cause heart attacks, strokes, headaches, ruin your kidneys, erectile dysfunction and shrink your brain.Before you start testosterone replacement or an exercise program, it is very important to get your blood pressure under control. This is done through diet, stress management, lowering your salt intake and/or the use of medications. It is a good idea to invest in a home-based blood pressure machine. One usually can be purchased at most pharmacy chains and cost under US$50. Some, like the OMRON HEM-780, can measure blood pressure easily and keep track of changes with time. Take measurements twice a day until you gain control of your blood pressure again. It is important to have your blood pressure measured during the first month of treatment to ensure that it does not increase with testosterone. The good news is that replacement doses are much less associated with this problem. More serious risks for hypertension are associated with the high testosterone doses associated with performance-enhancing use. NOTE: Some natural ways to decrease blood pressure are decreasing your salt intake, exercising, keeping a normal body weight for your height, managing stress, and engaging in meditation and yoga. "Erection-friendlier" blood pressure medications like ACE (angiotensin converting enzyme) inhibitors, renin inhibitors, ARB’s (angiotensin II receptor blockers), and combinations of them may be required for men who cannot maintain a blood pressure reading under 130/80 mm Hg. Avoiding Enlarged Breast (Gynecomastia)Yes, I am talking about breast appearance in men, not women. Gynecomastia is a benign enlargement of the male breast resulting from a growth of the glandular tissue of the breast. It is defined clinically by the presence of a rubbery or firm mass extending concentrically from the nipples. Men who start experiencing this problem complain of pain and tenderness around the nipple area. Gynecomastia is caused by higher than normal blood levels of estradiol, a metabolite of estrogen. As discussed earlier in the book, testosterone can convert into estradiol, DHT, and other metabolites. Men with higher amounts of the enzyme aromatase usually have this problem even at lower doses of testosterone. Growth of this glandular tissue is influenced by a higher fat percentage, older age, excessive alcohol intake, and the use of certain medications. Gynecomastia usually occurs early in testosterone replacement in those who experience this side effect.In several studies on testosterone replacement, only a very small percentage of people receiving testosterone experience growth of breast tissue. In one HIV-specific study conducted by Dr. Judith Rabkin in New York, she reported that out of 150 men enrolled in the study, two men experienced this adverse reaction. Gynecomastia is much more common among those who use high testosterone doses, such as bodybuilders (they call this "gyno" or "bitch-tits"). How do you manage gynecomastia if it does occur? Lowering the testosterone dose had not proven helpful for the two patients in Dr. Rabkin’s study. The use of antiestrogens, such as tamoxifen 10 mg twice daily, with lower doses of testosterone has been effective. Gynecomastia can become permanent if the condition lasts very long although it may reduce in size when the androgen use is discontinued. In the absence of resolution, surgical correction may be necessary in severe cases. For men who experience enlarged breast size, doctors usually check estradiol levels to determine whether too much testosterone is being converted into estrogen. I do not believe that routine measurement of estrogen is needed for men who have no symptoms of high estrogen (mainly breast tissue enlargement and water retention). For those who have higher than normal estrogen, doctors usually prescribe an antiestrogen medication. One such regimen is anastrozole at 1 mg/day during the first week until nipple soreness and breast enlargement disappear. The dose is then lowered to 0.25 mg a day, or 1 mg twice a week. A warning: Bringing estrogen down to very low levels could cause health problems in men in the long run. Hair/skin quality and health, brain function, bone density, and other important factors may be greatly influenced by estrogen. However a 12-week study in men using anastrozole at 1 mg a day and 1 mg twice a week found no changes in bone metabolism markers. The normal production ratio of testosterone to estrogen is approximately 100:1. The normal ratio of testosterone to estrogen in the circulation is approximately 300:1. Estrogen (measured as estradiol) should be kept at 30 picograms per milliliter (pg/mL) or lower. As men grow older or as they gain a lot of fat mass, their estrogen blood levels increase, even to levels higher than that of postmenopausal women. Medications and Products That Can Cause GynecomastiaA number of medications have been reported in the medical literature to cause gynecomastia due to decreases in testosterone, increases in estradiol, or both. These include:
Does Testosterone Suppress the Immune System?This question is raised out of the confusion over the use of the term "steroid." When somebody is having pain or inflammation and their physician prescribes them a "steroid" or something "steroidal", they are prescribing a corticosteroid (like prednisone) to decrease inflammation. These can have an immunosuppressive effect (sometimes its intended). The "steroid" that you hear about from the media when they are talking about use and abuse by athletes refers to an anabolic steroid (like testosterone). The similarities largely end with their street names.Some in vitro and animal data do suggest that high dose testosterone could be immune suppressive. No such immunosuppressive effect is seen when testosterone was added at replacement concentrations. Several studies using testosterone alone or on combination with oxandrolone or nandrolone in HIV-positive immune compromised patients have found no immune suppressive effect. |
Read more from this MESO-Rx article at:http://www.mesomorphosis.com/articles/vergel/testosterone-replacement-therapy.htm#ixzz1c6sBowuV
Sunday, October 9, 2011
FDA Approves Cialis to Treat Benign Prostatic Hyperplasia
October 6, 2011 -- The U.S. Food and Drug Administration today approved Cialis (tadalafil) to treat the signs and symptoms of benign prostatic hyperplasia (BPH), a condition in which theprostate gland becomes enlarged, and for the treatment of BPH and erectile dysfunction (ED), when the conditions occur simultaneously. Cialis was approved in 2003 for the treatment of ED.
Common symptoms of BPH include difficulty in starting urination and a weak urine stream; a sudden urge to urinate; and more frequenturination including at night.
The severity of symptoms of BPH can be measured using the International Prostate Symptom Score (IPSS). In two clinical trials, men with BPH who took 5 milligrams (mg) of Cialis once daily experienced a statistically significant improvement in their symptoms of BPH compared to men who were treated with placebo. The trials based their findings on a reduction in total IPSS scores.
In a third study, men who experienced both ED and BPH and who took 5 mg of Cialis once daily had improvement in both their symptoms of BPH and in their ED compared to men who were treated with placebo. The improvement in ED was measured using the Erectile Function domain score of the International Index of Erectile Function.
“BPH can have a big impact on a patient’s quality of life,” said Scott Monroe, director of the Division of Reproductive and Urologic Products in the FDA’s Center for Drug Evaluation and Research. “A large number of older men have symptoms of BPH. Cialis offers these men another treatment option, particularly those who also have ED, which is also common in older men.”
Cialis should not be used in patients taking nitrates, for example nitroglycerin, because the combination can cause an unsafe decrease in blood pressure. Also, the use of Cialis in combination with alpha blockers for the treatment of BPH is not recommended because the combination has not been adequately studied for the treatment of BPH, and there is a risk of lowering blood pressure.
The FDA has approved eight other drugs to treat symptoms of BPH: Proscar, (finasteride), Avodart (dutasteride), Jalyn (dutasteride plus tamsulosin), and the alpha blockers: Hytrin (terazosin), Cardura (doxazosin), Flomax (tamsulosin), Uroxatral (alfuzosin) and Rapaflo (silodosin).
Cialis is manufactured by Indianapolis-based Eli Lilly and Co.
Source: FDA
Posted: October 2011
Monday, August 1, 2011
Changes in Prostate Specific Antigen in Hypogonadal Men After 12 Months of Testosterone Replacement Therapy: Support for the Prostate Saturation Theory
Those who start at low baseline testosterone had the largest PSA increases. That makes sense since low levels of testosterone reduce prostate volume and prostatic specific antigen to levels under the expected median for a specific age. PSA levels normalized after the first month on the gel.
J Urol. 2011 Jul 23. [Epub ahead of print]
Changes in Prostate Specific Antigen in Hypogonadal Men After 12 Months of Testosterone Replacement Therapy: Support for the Prostate Saturation Theory.
Source
Scott Department of Urology, Baylor College of Medicine, Houston, Texas.
Abstract
PURPOSE:
We measured prostate specific antigen after 12 months of testosterone replacement therapy in hypogonadal men.
MATERIALS AND METHODS:
Data were collected from the TRiUS (Testim® Registry in the United States), an observational registry of hypogonadal men on testosterone replacement therapy (849). Participants were Testim naïve, had no prostate cancer and received 5 to 10 gm Testim 1% (testosterone gel) daily.
RESULTS:
A total of 451 patients with prostate specific antigen and total testosterone values were divided into group A (197 with total testosterone less than 250 ng/dl) and group B (254 with total testosterone 250 ng/dl or greater). The groups differed significantly in free testosterone and sex hormone-binding globulin, but not in age or prostate specific antigen. In group A but not group B prostate specific antigen correlated significantly with total testosterone (r = 0.20, p = 0.005), free testosterone (r = 0.22, p = 0.03) and sex hormone-binding globulin (r = 0.59, p = 0.002) at baseline. After 12 months of testosterone replacement therapy, increase in total testosterone (mean ± SD) was statistically significant in group A (+326 ± 295 ng/dl, p <0.001; final total testosterone 516 ± 28 ng/dl) and group B (+154 ± 217 ng/dl, p <0.001; final total testosterone 513 ± 20 ng/dl). After 12 months of testosterone replacement therapy, increase in prostate specific antigen was statistically significant in group A (+0.19 ± 0.61 ng/ml, p = 0.02; final prostate specific antigen 1.26 ± 0.96 ng/ml) but not in group B (+0.28 ± 1.18 ng/ml, p = 0.06; final prostate specific antigen 1.55 ± 1.72 ng/ml). The average percent prostate specific antigen increase from baseline was higher in group A (21.9%) than in group B (14.1%). Overall the greatest prostate specific antigen was observed after 1 month of treatment and decreased thereafter.
CONCLUSIONS:
Patients with baseline total testosterone less than 250 ng/dl were more likely to have an increased prostate specific antigen after testosterone replacement therapy than those with baseline total testosterone 250 ng/dl or greater, supporting the prostate saturation hypothesis. Clinicians should be aware that severely hypogonadal patients may experience increased prostate specific antigen after testosterone replacement therapy.
Copyright © 2011 American Urological Association Education and Research, Inc. Published by Elsevier Inc. All rights reserved.
Subscribe to:
Posts (Atom)




